9.1.1 Cutaneous Anatomy and Physiology
Anatomy
Three layers: the epidermis, the dermis and the subcutis with fascia.
Epidermis: germinative pool of keratinocytes (KC) and differentiating KC`s. Substructured into the basal membrane, stratum basale (dividing stem cells), stratum spinosum, stratum granulosum and stratum corneum. Melanocytes, Langerhans cells and Merkel cells.
Dermis: fibroblasts producing a rich extracellular matrix (collagen and elastic fibers), adnexal structure associated muscles, dermal dendritic cells, mast cells, Merkel cells, upper and lower vessel pool, apocrine and eccrine glands and different nerve types.
Subcutis: connective tissue and adipose tissue including vessels and immune surveillance cells.
Fascia
Skin glands: Eccrine sweat glands (palms and soles), apocrine sweat glands (axillae, areola and nipples, perianal region and genitalia) produce the sweat, sebaceous gland follicles, hair follicles with terminal hair and vellus hair follicles.
Read more
The skin is the largest organ of the body. It protects against external biological, chemical and physical assaults, and plays a role in thermic and water loss regulation, endocrine function, sensory perceptions and immuno surveillance. The human skin can be divided into three layers; the epidermis, the dermis and the subcutis with fascia.
The uppermost layer of the skin, the epidermis, is an organized, stratified epithelium with appendages (hair follicles, sweat and sebaceous glands) which project deep into the dermis.
The Epidermis is placed on the basal membrane, and is built up by continuously dividing cells, that maturate, undergo a special form of apoptosis and migrate towards the exterior. The epidermis can be subdivided into the basal membrane, a germinative pool of keratinocytes in stratum basale (dividing stem cells), stratum spinosum, stratum granulosum and stratum corneum where keratinocytes lose their nucleus and finally desquamate invisible.
The epidermis is a perpetually regenerating tissue, that must maintain a constant number of cells. It is expressing a range of pathogen-associated molecular pattern (PAMP) receptors and cytokine receptors. This maintenance depends on the ability of keratinocytes to undergo terminal differentiation and programmed apoptosis. Stem cells located in the skin are responsible for continual regeneration, wound healing, and differentiation of different cell lineages of the skin.
It forms the barrier layer of the skin, that prevents entrance of toxic and allergic substances and microorganisms, but also prevents the loss of water and electrolytes.
Keratinocytes synthesize keratin, a fibrous intermediate filament arranged in an alpha-helical coil pattern. Bundles of keratin filaments converge and terminate at the plasma membrane forming intercellular attachment plates known as desmosomes. Each epidermis layer has distinct morphologic and biochemical features, suggesting different roles in skin barrier function. Keratinocytes in the basal layer are responsible for the regeneration of the epidermis and are characterized by expression of keratins 5 and 14 (KRT5 and KRT14). KRT1 and KRT10 are more prominently expressed in the spinous layer. Gap junctions are another type of junction between keratinocytes.
Basal layer (stratum basale) is composed of keratinocytes attaching to the basal membrane with their long axis perpendicular to the dermis. These cells form a single layer. Some of them have the potential to divide and to migrate upstream to the external part of the epidermis.
Squamous cell layer (stratum spinosum) is composed of keratinocytes that become flatter as they move to the surface. They contain lamellar granules, membrane bound organelles containing glycolipids, phospholipids, sterols and acid hydrolases. The name comes from the spine-like aspect of the numerous desmosomes.
Granular layer (stratum granulosum) is composed of flattening cells with keratohyalin in their cytoplasm. Keratohyalin granules are basophilic and irregular. They play an important role for the formation of the interfibrillary matrix that holds keratin filaments together.
Cornified layer (stratum corneum) is composed of corneocytes, large, flat horny cells that have lost their nuclei during terminal differentiation. They are rich in proteins and low in lipids and provide mechanical protection and a barrier for foreign substances and to prevent water loss.
The same layers as in the epidermis can be found in the hair follicle, but these shafts penetrate the deeper dermis. The nails are also skin appendages, and have a similar structure to the hair follicles.
Epidermis also harbours melanocytes, Langerhans cells and Merkel cells.
Melanocytes reside in the basal layer of the epidermis where they form the epidermal melanin units as a result of the relationship between one melanocyte and 30-40 associated keratinocytes. The ratio of melanocytes to keratinocytes is 1: 7-10 in the epidermal basal layer (average melanocyte density is about 1.500 cells/mm2). Recent Research has shown no obvious differences in melanocyte density between the sexes or among people of different colors or races, but the melanocyte density can differ according to age, body part, and UV irradiation.
Melanocytes are dendritic cells that synthesize and secrete the pigment melanin. They are derived from neural crest cells and typically migrate to the epidermal-dermal junction during embryonic development, although a few can be found in the dermis. Dendritic extensions of the melanocytes are in contact with keratinocytes. Melanocytes produce melanin in rounded, membrane-bound organelles known as melanosomes, and transfer it to keratinocytes. Darker skin is related to the greater production of melanosomes, their larger size and slower rate of degradation. According to a recent Nature Communication pecific miRNAs associated with exosomes released from keratinocyte modulate human melanocyte pigmentation by enhancing the expression of proteins associated with melanosome maturation and trafficking. Caveolae in melanocytes are modulated by ultraviolet radiations and keratinocytes-released factors, like miRNAs. Preventing caveolae formation in melanocytes increases melanin pigment synthesis through upregulation of cAMP signaling and decreases cell protrusions, cell–cell contacts, pigment transfer and epidermis pigmentation. Increased ultra violet light exposure induces an increase in melanogenesis and in melanosome transfer to keratinocytes. Melanosomes aggregate above the nucleus and protects genetic information from radiation damage.
Merkel cells are mechanoreceptors attached to basal keratinocytes by desmosomal junctions. They are found in sites of high tactile sensitivity such as digits and lips.
Langerhans cells are dendritic cells deriving from the bone marrow that migrate to a suprabasal position in embryonic development and recirculate throughout life. They represent 3-7% of epidermal cells. Langerhans cells recognize and process antigens encountered in the epidermis. These cells then undergo maturation that stimulates their migration capacities. They can migrate to the local lymphnode to present antigens.
Dermis is located below the epidermis. It is composed mainly of fibroblasts, producing a rich extracellular matrix of proteoglycans, glycosaminoglycans, collagen, elastic fibres, vessels, glands and nerves, adnexal structure associated muscles, dermal dendritic cells, mast cells, Merkel cells, upper and lower vessel pool, apocrine and eccrine glands and different nerve types.
Dermis is composed of two layers, the papillary layer with papillae extending into the epidermis, and below the reticular layer constituted of looser connective tissue.
The subcutis or hypodermis is built up by connective tissue and fat, vessels and immune surveillance cells, and reaches the muscle fascia. It harbors adipose tissue for fat storage and protection.
The human skin has different kinds of glands.
Eccrine sweat glands consist of long curved secretory and excretory tubules and can be found almost everywhere on the body, very densely on the palms and soles.
Apocrine sweat glands are mostly found in the axillae, areola and nipples, perianal region and genitalia. Their orifice is at the uppermost part of the hair follicle canal. Pheromones are released to the surface of the skin. The lactiferous (breast) glands are modified apocrine glands. Sexual hormones influence the function.
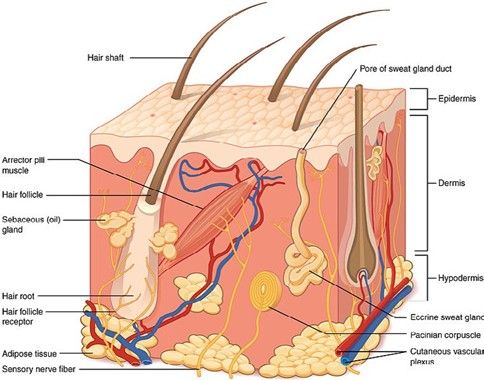
Sebaceous glands are an endocrine organ by itself. Smaller sebaceous glands are also associated to the hair follicles with terminal hair and vellus hair follicles. They produce a variety of lipids and by a regulated form of apoptosis they release the sebum to the infundibulum that oils the hair and contribute to the lipid content of the stratum corneum. Androgens and growth factors regulate the glands.
Hair follicle density varies according the location on the surface of the body. The highest hair follicle density and percentage of follicular orifices on the skin surface are found on the forehead, whereas the highest average size of the follicular orifices is found in the calf region, although the calf region shows the lowest hair follicle density. Every body region shows its own hair follicle characteristics. Terminal hair follicles are at the scalp, beard, axillary and pubic region or trunk and differ according to gender, age, hormone receptors and isoenzyme distribution.
The dermal vasculature is composed of two intercommunicating plexuses: the subpapillary or superficial plexus, at the junction of papillary and reticular dermis, and the lower plexus at the dermal- subcutaneous interface.
Thermal regulation
Skin vasculature plays a key role in thermal regulation. Glomus cells help to regulate the diameter of the vessels so that the higher or lower amount of blood can heat or cool down the skin. The eccrine glands produce sweat when stimulated by cholinergic nerves (stress reaction, temperature cooling down the skin), which cools the skin physically by evaporation. An anchoring muscle of the hair follicle (musculus arrector pili) can produce some heat by moving the follicle upward.
Physical protection
Epidermis (especially the stratum corneum): provides protection from evaporation of water and physical stress.
Dermis: protects the skin against tears and shear forces and provides elasticity.
Subcutis: fat tissue can absorb and distribute physical harm.
Read more
The subcutis, containing fat tissue can absorb and distribute physical harm.
The dermis, thanks to its dense collagen network, plays an essential role by protecting the skin against tears and shear forces and provides an elastic structure to keep the shape of the skin.
The epidermis, especially the stratum corneum, builds the outermost layer of the skin, providing protection from evaporation of water and physical stress, but also helps to keep the roughness of the skin. The stratum corneum is particularly thicker on the palms and soles, where it is exposed to more physical usage and thinner on the lips or periorbital region
Protection against chemical injury
Stratum corneum: corneocytes (keratinocyte envelopes) and sebum help the skin to resist various kinds of chemical injuries and water.
Read more
The stratum corneum consists of dead cells, “keratinocyte envelopes” that consist mainly of filaggrin, keratin protein and amino acids. Between the keratinocytes, the sebum, a lipophilic material fills the space, similarly to a wall that consists of bricks and mortar. This mixture of hydrophobic and hydrophilic substances helps the skin to resist against various kinds of chemical injuries and water.
This explains also why skin care products containing both lipidic and hydrophilic structures should be used.
Photoprotection
Melanocytes produce melanin and transfer them in vesicles to the surrounding keratinocytes. Melanin absorbs ultraviolet (UV)-radiation and thereby protect genetic material. KC produce ROS absorbers and repair enzymes against DNA damage.
Read more
Melanocytes, located on the basal membrane, produce melanin and transfer them in vesicles to the surrounding keratinocytes. The keratinocytes phagocyte these vesicles (granules) and group them around their nucleus. The two kinds of melanin, eumelanin and pheomelanin absorb ultraviolet (UV)-radiation but also visible light and protect thereby the genetic material that may be damaged by UV radiation. Although the melanin production is genetically determined it can be induced by external (UV, light) or internal (hormones, inflammation) stimuli. KC produce ROS absorbers and repair enzymes against DNA damage.
Sensory function
The skin is one of the most important sensory organs: nerves and receptors such as nociceptors (pain and itch receptors) and Merkel cells (mechanoreceptors) are responsible for the touch.
Read more
The skin is one of the most important sensory organs. Various kinds of nerves reach up to the upper dermis. Sensing nerves are organized by dermatomes, which can be observed in Herpes zoster infections. Receptors of the skin include nociceptors (pain and itch receptors) or free nerve endings, that are responsible for the sensing of heat, cold, pain, touch, itch and motion. Cutaneous mechanoreceptors include Ruffini’s end organ (skin stretch), end-bulbs of Krause (cold), Meissner’s corpuscle (changes in texture, slow vibrations). Pacinian corpuscules are onion-shaped deeper mechanoreceptors responsible for the sensation of vibration. Other types of receptors are thermoreceptors and chemoreceptors. Merkel cells are neuroendocrine cells that interact with the mechanoreceptors in complexes called hair disks
Immune function
Most of the lymphocytes in the skin, other leukocytes, mast cells, and macrophages. Epidermis: Langerhans cells (antigen-presenting cells); keratinocytes (epithelial cells with immune properties), dendritic epidermal T lymphocytes, resident memory T cells that may serve as a primitive T-cell immune surveillance system; and immunogenic melanocytes. Dermis: most of the lymphocytes in the skin, other leukocytes, dermal dendritic cells, mast cells and macrophages.
Subcutis: immune surveillance reservoir and progenitor cells for wound healing.
Read more
The skin is more than a physical barrier: it is an active immune organ. Immune responses in the skin involve different immune-competent cells and soluble molecules including cytokines. The dermis contains lymphatic and blood vessels and most of the lymphocytes in the skin, other leukocytes, dermal dendritic cells, mast cells, and macrophages. Although the epidermis has no direct access to the blood or lymphatic circulation, it contains immune-competent cells:
Langerhans cells (antigen-presenting cells);
keratinocytes (epithelial cells with immune properties), dendritic epidermal T lymphocytes, resident memory T-cells that may serve as a primitive T-cell immune surveillance system; and
melanocytes (pigment cells with immune properties).
Langerhans cells are able to detect antigens and migrate to the surrounding lymph nodes to present these antigens to T-cells, which activates the T-cells and stimulates their migration to the skin.
The subcutis is a reservoir for immune surveillance cells and for progenitor cells for wound healing. Melanocytes are immunogenic due to the contents of their melanosomes, generating the complex radical scavenging molecule melanin in a process that involves melanogenic enzymes and structural components, including tyrosinase, MART-1, gp100, TRP-2 and TRP-1. These molecules are also targets of the immune response in both vitiligo and melanoma. The immunogenicity of melanosomal proteins can be explained by the dual role of melanosomes, involved both in melanin synthesis and processing of exogenous antigens. Melanocytes are also capable of presenting antigens in the context of MHC class II.



 English
English
 German
German
 French
French
 Italian
Italian
 Spanish
Spanish
 Portuguese
Portuguese
 Chinese
Chinese
 Lithuanian
Lithuanian

Comments
Be the first one to leave a comment