10.2.1 Chomoblastomycosis
ICD-11
1F24
Synonyms
Medlar bodies; muriform bodies; copper pennies.
Epidemiology
Affecting mostly adult male agricultural workers in the rural tropical and subtropical areas of the world.
Definition
Chronic granulomatous infection of the skin and subcutaneous tissue caused by several different brown pigment-producing (dematiaceous) fungi.
Aetiology & Pathogenesis
A large number of dematiaceous, i.e.brown pigment producing, fungi can cause the disease, the most common of which are Cladosporium carrionii, Phialophora verrucosa, and Fonsecaea pedrosoi, present in wood an soil.
Signs & Symptoms
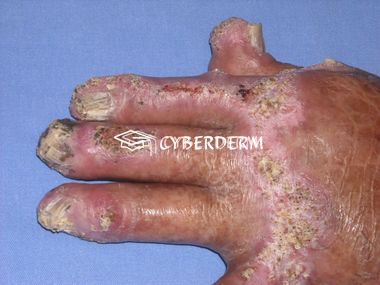
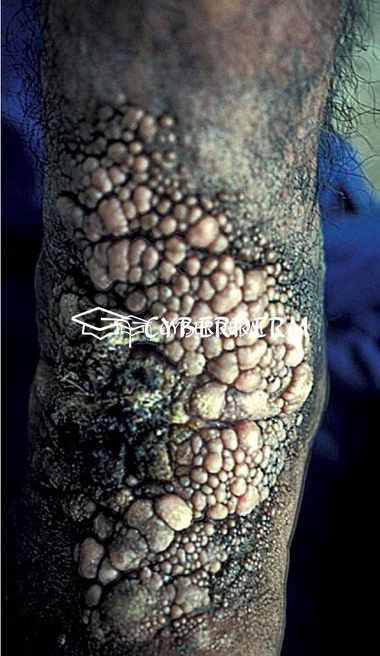
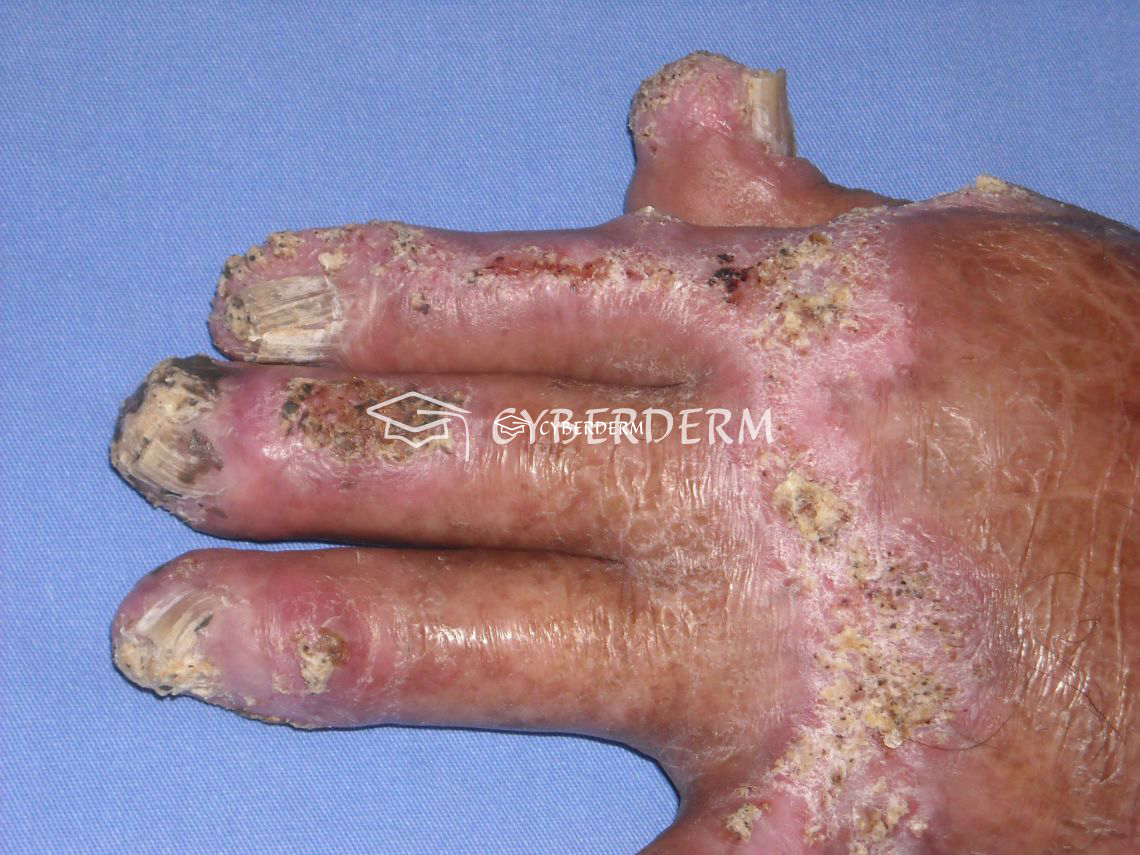
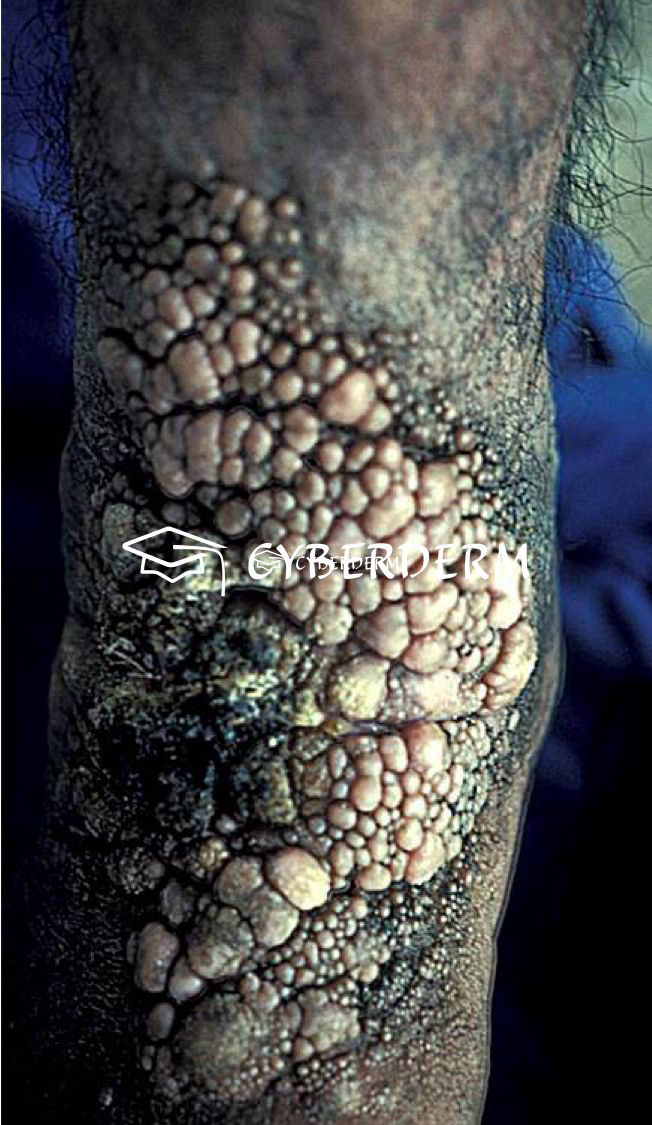
Localized, slowly growing and peripherally extending, warty cauliflower-like plaques, which may ulcerate. Sclerotic bodies are extruded tranaepidermally, appearing as black dots. Large hyperkeratotic and ulcerating masses may form. The lesion is usually painless. Sometimes lymphatic spread due to scratching result in the sporotrichoid pattern. Hematogenous dissemination with brain abscesses is very rare.
Localisation
Areas exposed to trauma.
Classification
None.
Laboratory & other workups
Microbiology; 10% KOH.
Dermatopathology
Marked pseudoepitheliomatous hyperplasia of the epidermis. Transepidermal elimination of fungal cells, which are in the stratum corneum. Foreign-body granuloma with isolated microabscesses. In the dermis, a granuloma composed of epithelioid cells and Langhans giant cells is visible. The golden-brown fungal elements are visible as thick-walled, single, or multicelled clusters, forming sclerotic or muriform bodies.
Course
Chronic, but curable. The prognosis depends on the size of the lesions and the immune status of the patient. Long-standing cases can spread over joints and lead to lymphatic involvement and elephantiasis. Disseminated disease, with the involvement of the central nervous system, has the worst prognosis.
Complications
Ulceration, secondary bacterial infection, lymphedema resulting in elephantiasis. Malignant transformation to squamous cell carcinoma is rare.
Diagnosis
Clinical feature, histologic and microbial findings.
Differential Diagnosis
Other verrucous lesions: tuberculosis verrucosa cutis, verruca vulgaris, blastomycosis, Yaws, verrucous hemangioma, hypertrophic lichen planus, lupus vulgaris. Sporotrichosis in sporotrichoid type. Psoriasis.
Prevention & Therapy
Prevention of trauma.
Best results are achievable in small lesions with surgery, cryotherapy or electrodessiccation in combination with antifungal therapy: itraconazole 200 to 400 mg/day or terbinafine, 250 to 500 mg/day given for a period varying from 6 months to a year or more. Flucytosine alone or combined with amphotericin and oral supersaturated potassium iodide solution are additional options.
Special
Best management is by an interprofessional team, including an infectious disease consultant, surgeon, emergency department physician, wound care nurse, and an internist.
Review Articles
- G. Kurien, K. Sugumar, V. Chandran: Chromoblastomycosis
- A.C. de Brito, M. de Jesus Semblano Bittencourt: Chromoblastomycosis: an etiological, epidemiological, clinical, diagnostic, and treatment update*
- O. Lupi, S.K. Tyring, M.R. McGinnis: Tropical dermatology: Fungal tropical diseases
- F. Queiroz-Telles, S. de Hoog, D.W. C. L. Santos, et al.: Chromoblastomycosis



 English
English
 German
German
 French
French
 Italian
Italian
 Spanish
Spanish
 Portuguese
Portuguese
 Chinese
Chinese
 Lithuanian
Lithuanian

Comments
Be the first one to leave a comment